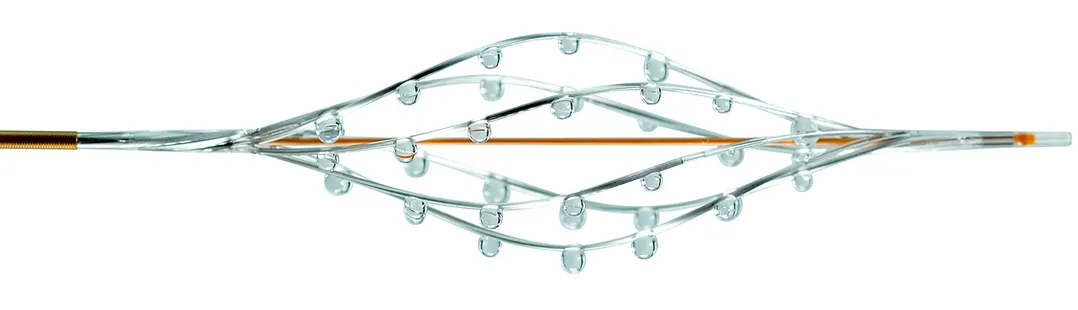
Marked reduction in segmental and main pulmonary artery occlusions shown in NIH-sponsored RESCUE trial with the BASHIR™ Endovascular Catheter in Patients with Intermediate Risk Acute Pulmonary Embolism
NEW BRITAIN, PA (March 6, 2023). Robert A. Lookstein MD, Executive Vice Chair, Diagnostic, Molecular and Interventional Radiology at the Icahn School of Medicine at Mount Sinai Hospital, New York, today presented the results of an important sub-analysis of Thrombolex’s National Heart, Lung and Blood Institute (NHLBI) – sponsored RESCUE trial during the Late Breaking Trial Session at the Society for Interventional Radiology (SIR) annual meeting in Phoenix. The core laboratory analysis of this investigational device exemption (IDE) trial demonstrated that pharmaco-mechanical catheter-directed thrombolysis (PMCDT) therapy using the BASHIR™ Endovascular Catheter from THROMBOLEX led to a significant reduction in segmental arterial occlusions (71%, p<0.0001)) which correlated with the reduction in (right ventricular to left ventricular (RV/LV) ratio (p= 0.0026). There was also a significant reduction in main pulmonary artery (PA) occlusions (61%; p<0.0001) but this did not correlate significantly with the reduction in RV/LV ratio. This reduction in occlusions of not only the main PAs but also the segmental arteries explains why the overall reduction in PA obstruction as assessed by the refined Modified Miller Index is greater with the BASHIR™ Endovascular Catheter than what has been reported in other contemporary thrombectomy or thrombolysis trials for the treatment of acute pulmonary embolism (PE). The magnitude of effect of these other treatments on segmental arterial occlusions has not previously been reported.
The RESCUE trial is a prospective, multicenter trial evaluating the BASHIR Catheter in 109 patients with intermediate risk acute PE at 18 sites in the United States. The BASHIR™ Catheter was used to deliver 7mg of recombinant tissue plasminogen activator (r-tPA) into each PA over a 5-hour infusion period. The primary efficacy endpoint was the core lab-assessed change in the CTA-derived mean RV/LV diameter ratio at 48 hours, and the primary safety endpoint was serious adverse events, including major bleeding at 72 hours. The median device placement time was 15 minutes and length of hospital stay was 2.8 days.
“The RESCUE trial demonstrated rapid resolution of obstruction in the main and especially segmental arteries, with less than a 1% major bleeding rate. It is imperative that future PE trials assess the reduction in obstruction in more distal PAs since it has been shown that both the degree of residual PA obstruction and reduction in pulmonary vascular volumes, presumably due to reduced PA inflow, are significant predictors of late PE-related mortality. This novel approach with the BASHIR™ catheter and low-dose tPA represents a major advance in the treatment of acute PE,” said Dr Robert Lookstein.
“We are pleased to be able to share this important new information from our RESCUE trial and thank all those who made this possible, especially our physician investigators and their patients. We would also like to thank the NIH and the Commonwealth of Pennsylvania Department of Health for their support,” said Brian G. Firth, MD, PhD, FACC, Chief Scientific Officer of Thrombolex and Principal Investigator of the NHLBI- funded SBIR grant to THROMBOLEX.
About THROMBOLEX
Founded in 2016, THROMBOLEX is engaged in the design, development and distribution of innovative endovascular catheters used in interventional procedures, particularly in pharmaco-mechanical catheter-directed thrombolysis (PMCDT) in patients who suffer from arterial and venous thromboembolic (VTE) conditions. The Company is currently marketing seven (7) different FDA cleared devices that are all based on the BASHIR™ Endovascular Catheter platform technology. The BASHIR™ Endovascular Catheter has not been cleared by the FDA for the treatment of acute pulmonary embolism.
For More Information: Please contact Dr. Brian Firth, Chief Scientific
Officer brian@thrombolex.com or visit our website www.thrombolex.com